In this article, I’ll provide a brief overview of Kohlberg’s moral theory and how it can help medical interpreters make ethical decisions. I’ll use examples of common challenges and ethical dilemmas that interpreters face on the job to examine them through Kohlberg’s eyes. I believe that understanding Kohlberg’s theory can improve moral reasoning flexibility, increase critical thinking, and serve as a reflection tool for medical interpreters and many other professions. Throughout this article, I’ll refer to two different scenarios: Heinz Steals the Drug, the scenario used in Kohlberg’s research, and Interpreter Stand By, a real-life interpreting scenario to which I will apply Kohlberg’s levels and stages.
What’s Kohlberg’s Theory of Moral Development?
Lawrence Kohlberg was a twentieth-century American psychologist best known for his theory of moral development. He built on Jean Piaget’s research on moral judgment and identified six stages of moral reasoning that people go through as they age.
Kohlberg reached this conclusion after conducting research in which he interviewed children and teenagers who were presented with moral dilemmas through stories and asked whether or not they thought a particular behavior was right or wrong. Kohlberg was more interested in the thinking process behind their moral judgment than in their response.
The Heinz dilemma is one of the best-known stories Kohlberg told children during his research.
Heinz Steals the Drug
‘’In Europe, a woman was near death from a special kind of cancer. There was one drug that the doctors thought might save her. It was a form of radium that a druggist in the same town had recently discovered.
Kohlberg (1963) p. 12
The drug was expensive to make, but the druggist was charging ten times what the drug cost him to make. He paid $200 for the radium and charged $2,000 for a small dose of the drug.
The sick woman’s husband, Heinz, went to everyone he knew to borrow the money, but he could only get together about $1,000 which is half of what it cost. He told the druggist that his wife was dying and asked him to sell it cheaper or let him pay later. But the druggist said: “No, I discovered the drug and I’m going to make money from it.” So Heinz got desperate and broke into the man’s store to steal the drug for his wife. Should the husband have done that?’’
The children were then asked whether Heinz should or should not have stolen the drug. Kohlberg classified their responses into the following moral reasoning levels and stages:
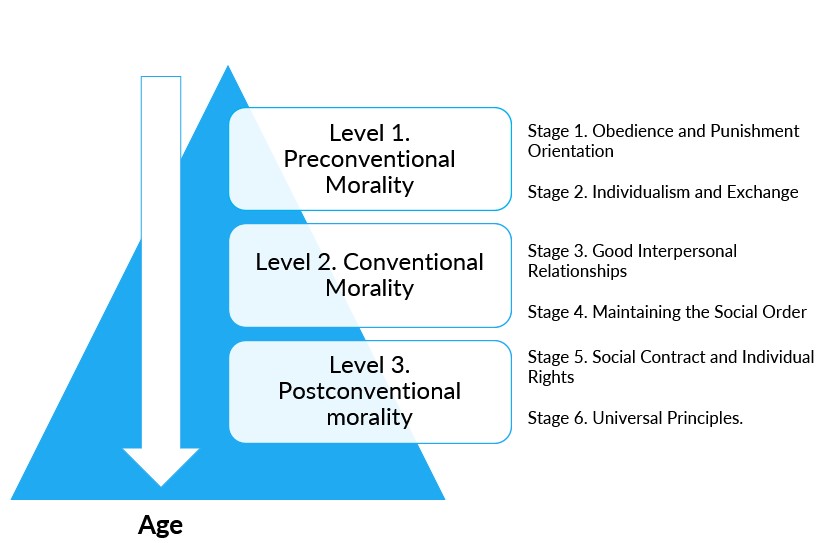
Level 1. Preconventional Morality.

Stage 1. Obedience and Punishment Orientation. Morality is imposed by figures of authority, and they hand down rules that children must follow in order to avoid punishment. A child may respond that Heinz should not have stolen the drug because it is against the law, and Heinz could face punishment. What the authorities allow and whether or not Heinz is punished determine whether or not an action is right or wrong. (Crain, 2014)
Stage 2. Individualism and Exchange. Children at this stage recognize that there are multiple points of view, not just the one handed down by authorities. As a result, each individual can select the viewpoint that best suits their needs or is personally satisfying. For example, a child may respond that Heinz could steal the drug if he wanted his wife to live, but he didn’t have to if he wanted to marry someone else. Children may also think in terms of “fair deals,” as in, “if you do something for me, I’ll do something for you.” For example, if Heinz steals the drug, his wife may someday repay the favor. (Crain, 2014)
Throughout this article, I’ll use the following interpreting scenario, “Interpreter Stand By,” and examine it from Kohlberg’s perspective at each stage. This can help internalize what each stage consists of and evaluate the interpreter’s behavior. Keep in mind that, at this point, I’m not saying what you, as an interpreter, should do in this situation. I’m only describing what an interpreter might think, say, or do in this situation, using each stage of moral reasoning.
Interpreter Stand By
A medical interpreter is interpreting over the phone for a Spanish-speaking patient and a primary care doctor. The doctor asks the interpreter to stand by and starts speaking in Spanish to the patient. However, the patient has a difficult time understanding the doctor since the doctor has limited Spanish proficiency. The interpreter notices this but remains on standby as the provider instructed.
Should the interpreter have remained on stand-by, or should they have done something else?
When answering this question using Level 1 reasoning, an interpreter would say that interpreters should follow the doctor’s instructions because doctors have more authority and expertise than patients and interpreters during a medical encounter. Doctors prescribe medications, educate patients, and give treatment; often, they have more information about a patient than interpreters because they have interacted with them more frequently over a longer period of time, and they call interpreters when necessary, so the provider is the person “in charge” of the encounter. As a result, interpreters should defer to them.
Furthermore, an agency may instruct its interpreters to always follow the medical provider’s instructions. Otherwise, the interpreter may receive a complaint from the doctor or fail their quality assurance review, which may result in a reduction in bonus benefits or work hours. To avoid these negative consequences, an interpreter could decide to stand by.
Level 2. Conventional Morality

Stage 3. Good Interpersonal Relationships. Children, now in their adolescence, move away from seeing morality as simple deals and the ‘’what is it in for me’’ position. Instead, they begin to value social approval from others and strive to be the “good boy” or “good girl” by living up to social expectations and rules of good behavior. In Heinz’s scenario, respondents could say that Heinz should have stolen the drug because that’s what a good husband would do to save his wife, or they could say that stealing is wrong and other people would think of Heinz as a criminal.
The interpreter’s perspective…
At this stage, an interpreter would consider what the professional community would expect a good interpreter to do. These expectations may vary depending on the community the interpreter is part of, but the interpreter will conform to those expectations, whatever they are.
Let’s say the interpreter is a member of a medical interpreting association, has taken several of their online webinars, and participates in Facebook group discussions about ethical dilemmas. They recall from conversations with colleagues that whenever someone in the encounter requests that you not interpret, the recommended action is to remind all parties of the interpreter’s responsibility to convey all messages accurately and completely. So the interpreter chooses to do so because that is what their community would consider a wise decision.
This interpreter can also consider how their intervention, or lack thereof, may affect their relationship with the patient and doctor. If the interpreter does not intervene, the patient may believe they were not assisted properly by the interpreter. If the interpreter does intervene and tell the doctor that their Spanish isn’t fluent enough, the doctor may interpret that as challenging their authority, and this could create conflict.
So, the interpreter “picks” sides. If one side is right, the other is wrong. For example, if the interpreter sides with the doctor, they believe the patient should have advocated for themselves, and if they side with the patient, they believe the provider is wrong for attempting to communicate in a language they’re not fully proficient in.
In summary, the interpreter’s actions are motivated by maintaining a good interpersonal relationship with either the patient or the doctor, and adhering to the rules of their community; they view things from a dualistic perspective (good or bad) and choose to be on the ‘’good’’ side.
One of my criticisms of this reasoning would be that it reinforces ‘’black and white’’ thinking and limits the interpreter’s ability to make better decisions, but I will go over all the objections to Kohlberg’s moral theory and how it applies to interpreters in a separate post.
Stage 4. Maintaining the Social Order. In this stage, the focus is placed on respecting the law and the authorities and fulfilling one’s duty to maintain the social order. If everyone broke the law when they felt like they had a good reason, we would live in chaos. Respondents in Stage 1 (Obedience and Punishment) may also say that stealing is wrong, but they cannot elaborate further than “it’s against the law,” whereas respondents in Stage 4 can see how Heinz’s actions affect society as a whole. (Crain, 2014)
An interpreter looking at this scenario from a Stage 4 perspective may think about established Codes of Ethics and Standards of Practice, as well as U.S. language access laws, from which they can conclude that the provider erred in refusing to communicate through the interpreter and speaking to the patient in Spanish, despite their limited language proficiency, and the interpreter erred in choosing to stand by instead of intervening to ensure accurate communication, for the following reasons:
- Not providing an interpreter to patients with Limited English Proficiency is considered language discrimination and prohibited under several U.S. laws (OCR, 2015)
- If all physicians spoke to the patient in a language they were not proficient in, medical care would be negatively impacted as doctors and patients wouldn’t be able to understand each other. This would result in poor communication that could lead to clinical errors and, potentially, malpractice lawsuits.
- Not communicating through an interpreter goes against established best practices by professional associations as well as physician and medical interpreters’ codes of ethics alike, such as those published by the AMA for physicians and the NCIHC, IMIA, and CHIA for medical interpreters.
Level 3. Postconventional morality

Stage 5. Social Contract and Individual Rights. While Stage 4 respondents respect the law and want to maintain social order, Stage 5 respondents recognize that laws can conflict with our moral outlook. They see laws as shared agreements, or “social contracts,” for the benefit of everyone in society rather than as unchangeable, rigid rules. Although different social groups may have different moral perspectives on the law, most people would agree on two points (Crain, 2014):
- There are certain basic rights that need to be protected. In Heinz’s case, some respondents may say that the wife’s right to life is more important than breaking the law.
- Democratic procedures can be used to change laws. For example, unfair laws can be changed by reaching a consensus through voting.
Moral reasoning is guided by ethical principles, such as justice and respect, that take precedence over society’s rules and laws. Individuals have internalized these ethical principles and follow them regardless of the punishment or rewards they may receive because ethical behavior is seen as the right thing to do in and of itself.
Stage 6. Universal Principles. An important difference between Stage 5 and Stage 6 individuals is that Stage 5 individuals only seek changes within the boundaries of the law, whereas individuals in Stage 6 have a commitment to justice that includes a responsibility to disobey unjust laws. There have been many important activists who broke the law for what we now consider just reasons, like Rosa Parks in racially segregated Alabama (U.S.), who was arrested for refusing to give up her bus seat to a white person as the law required.
Stage 6 individuals can see how laws can lead to unjust outcomes when a majority group votes for a law that hurts a minority group. Therefore, to make just decisions, one must be able to put oneself in other people’s shoes by adopting a ‘’neutrality mantle’’ and treating everyone fairly (Crain, 2014). For example, if the druggist in Heinz’s scenario were in the wife’s shoes, he wouldn’t want to be denied the medicine and have it valued more than his own life, so he would agree that Heinz’s wife should be saved. (Crain, 2014)
What would a post-conventional interpreter be like?

The following paragraphs are a description of what an interpreter on the post-conventional level would be like and how they would respond in the ‘’Interpreter Stand By’’ scenario:
The interpreter has very good knowledge of language access laws and standards of practice for medical interpreters, but they’re also aware that these are not set in stone; they can be changed to respond adequately to the needs of the population they serve and help ensure proper interpretation. This interpreter believes that these changes can be made by using the means provided by the government and organizations that help improve medical interpretation services.
At the same time, this interpreter knows that organizational and government processes alone sometimes aren’t enough to bring about change, so the interpreter’s practice is also guided by their independent understanding of what’s best for interpretation in medical encounters based on the four principles of medical ethics:
- Beneficence (do good)
- Non-maleficence (do no harm)
- Autonomy (the right of patients to make informed decisions about their care)
- Justice (treating all patients fairly)
When the interpreter sees that these principles are not respected, they feel a duty to correct this situation while keeping in mind the multiple perspectives on the issue.
For example, when this interpreter is put in the scenario ‘’Interpreter Stand By’’, they recognize that the doctor wanting to speak to the patient in a language they’re not fully proficient in is problematic because it puts the patient’s safety at risk by creating potential misunderstandings in communication that could lead to negative health outcomes. The doctor’s behavior also violates 3 ethical principles:
- Autonomy. The patient may be given wrong or inaccurate information about their treatment plan, medication, or any other clinical information, which hinders their ability to make informed decisions.
- Non-maleficence. The provider may be harming the patient if the language misunderstandings impact the patient’s health negatively. As an example, I will use the well-known case of Willie Ramirez, a baseball player in the 1980s who was misdiagnosed with having a drug overdose because doctors confused the words ‘’intoxicated’’ and ‘’intoxicado’’. Intoxicado means ‘’food poisoned’’ in Spanish. Doctors later on discovered Willie was having a stroke, but they did not provide prompt treatment. Unfortunately, Willie became quadriplegic as a result of this misdiagnosis due to an incorrect translation. (Health Affairs, 2008)
- Justice. If the doctor doesn’t communicate through a qualified interpreter when needed, the Spanish-speaking patient would have more difficulties understanding their clinical information and become more likely to suffer the negative consequences of medical errors due to mistranslations. This puts them at an unfair disadvantage when compared with their English-speaking counterparts, who are less likely to experience these problems.

This Stage 6 interpreter would disapprove of how the interpreter in the ‘’Interpreter Standby Scenario’’ decided not to intervene as this is against the ethical principles I mentioned above.
Additionally, this interpreter is also capable of putting themself in the doctor’s and patient’s shoes. They can see how doctors, in general, don’t mean to put the patient’s care at risk. Most likely, the doctor wants the medical encounter to go a little faster or is overconfident in their language skills; oftentimes, doctors are not aware of the complexities of language and interpretation, or the legal requirement to communicate through a qualified medical interpreter. The patient, on the other hand, may have found it difficult to voice their concerns, not only because of the language barrier, but also because the doctor is perceived as an authority figure, and they may not feel comfortable challenging their authority. The interpreter keeps these possibilities in mind to formulate their response.
The interpreter would respond by politely refusing to stand by. Instead, they give the doctor a short, convincing explanation of why it’s important to communicate through the interpreter, based on ethics, the law, and the agency or medical center’s policies as needed. For example, the interpreter could say, ‘’I apologize. I’m not allowed to stand by. As I’m connected to this call, I’m required, per agency policies and codes of ethics, to interpret for this encounter. I’d be more than happy to ask your questions to the patient to make sure everything is said accurately and completely and avoid any misunderstandings.’’ The interpreter would also be transparent with the patient and let them know what the doctor asked the interpreter to do and the interpreter’s response.
The doctor may or may not comply with the interpreter’s request. If they do, then the problem is solved, and the interpreting session can continue as usual. If they don’t, the interpreter can restate their request in a different way until they convince the doctor. But let’s assume that the doctor, after going back and forth with the interpreter, decides to hang up the phone and call a new interpreter. In that case, the interpreter feels responsible for reporting that doctor because they deem their behavior unethical. They make sure to report through the most appropriate channels, for example, the compliance or quality assurance departments in the medical center or the interpretation agency.
If the interpreter notices that, despite filing complaints, the issues persist or are ignored by the agency or medical center, they seek alternative solutions, such as filing a civil rights complaint with a higher authority, such as the U.S. Department of Health and Human Services. They could also advocate for good language access practices within their communities and professional organizations, or even start their own organization to solve one or more interpretation problems using all of the resources available to them.
Summary
In summary, Kohlberg’s theory of moral development divides moral reasoning into three levels that we progress through as we age: Preconventional, Conventional, and Postconventional levels. On the Preconventional level, individuals base their moral decisions on self-interest and following the rules of the authorities to avoid punishment.
On the Conventional level, the emphasis shifts to having good interpersonal relationships by doing what society expects of a good person and obeying the laws that maintain the social order. On the Postconventional level, individuals begin to consider changes in the law that would benefit society, and sometimes, even disobey the law when it violates certain ethical principles.
But how can we interpreters apply this knowledge in a way that’s meaningful to our jobs? Through practice exercises, this is what we do at InterpreMed’s Ethics Club! On Saturday, March 25th of 2023, at 1:00 p.m. EST, we will study Kohlberg’s moral theory in depth using real-life ethical dilemmas and interpreting scenarios while giving attendees solutions to respond to a variety of ethical dilemmas. The meeting will also be recorded for our members who can’t join live.
Join our Ethics Club and benefit from many of our interpreting resources by becoming a Pro, +Memory Club, or Master+Memory Club member at InterpreMed.com!
References
- Kohlberg, L. (1963). The development of children’s orientations toward a moral order: I. Sequence in the development of moral thought. Human Development, p.12
- U.S. Department of Health and Human Services, Office of Civil Rights (OCR) (2015) Discrimination on the Basis of Race, Color, or National Origin (including LEP), retrieved from https://www.hhs.gov/civil-rights/for-individuals/race/index.html
- Crain, William (2014). Theories of Development Concept and Application, 6th edition
- NCIHC (2005). National Standards of Practice for Interpreters in Health Care
